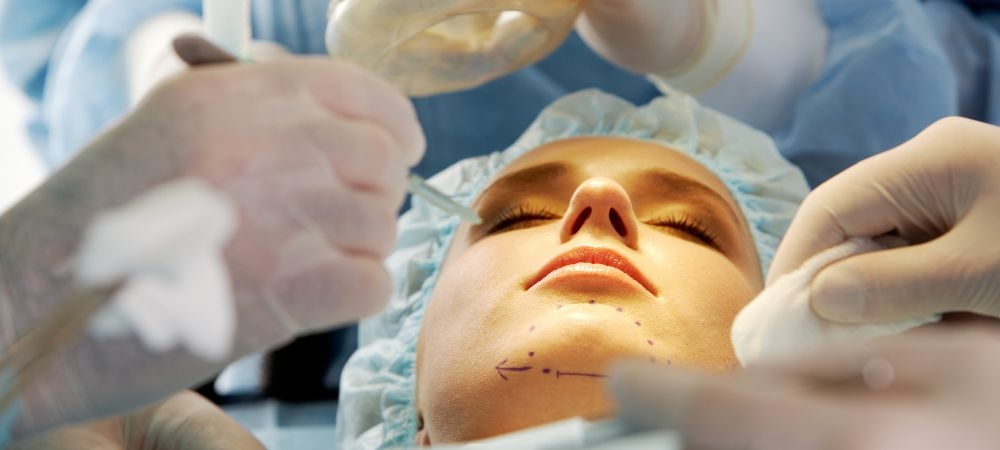

In Vitro Fertilization (IVF) is a sophisticated medical procedure designed to assist individuals and couples in conceiving a child when natural conception is challenging or impossible. The process begins with ovarian stimulation, where hormonal treatments are administered to encourage the ovaries to produce multiple eggs instead of the single egg typically matured during a natural cycle. This hormonal therapy, usually delivered through daily injections, promotes the growth of multiple follicles, each housing an egg. The development of these follicles is meticulously monitored through blood tests and ultrasounds to ensure optimal timing for the subsequent procedures. Once the follicles reach maturity, a final hormone injection is given to trigger ovulation, preparing the eggs for retrieval. Timing is crucial, as the eggs must be collected just before they are released from the ovaries. The egg retrieval procedure is performed under light sedation or anesthesia, where a healthcare provider uses a thin, hollow needle inserted through the vaginal wall to aspirate the mature eggs from the follicles. After retrieval, the eggs are carefully prepared and assessed in the laboratory.
Following retrieval, the fertilization of the eggs occurs in a laboratory setting. The eggs are combined with sperm, which can be done through conventional insemination, where sperm is added to the eggs and allowed to fertilize naturally, or through Intracytoplasmic Sperm Injection (ICSI), where a single sperm is injected directly into an egg. The choice between these methods often depends on specific fertility issues, such as sperm quality or quantity. After fertilization, the resulting embryos are cultured for several days, during which embryologists closely monitor their development and select the healthiest embryos for transfer. CureValue . Typically, embryos are cultured for 3 to 5 days until they reach the blastocyst stage, which is optimal for implantation.
The final step involves the embryo transfer, where one or more healthy embryos are placed into the uterus through a thin catheter inserted via the cervix. This procedure is generally painless and does not require anesthesia. After the transfer, hormone supplements may be prescribed to support the uterine lining and enhance the chances of successful implantation. Approximately two weeks after the embryo transfer, a pregnancy test is conducted to determine if the procedure was successful. If implantation occurs and the test is positive, further monitoring will ensure the health of the pregnancy. Conversely, if the test is negative, adjustments may be made, and the process can be repeated as necessary.
Overall, IVF is a highly controlled and intricate process involving hormonal treatments, meticulous handling of eggs and sperm, and careful embryo transfer, all aimed at maximizing the likelihood of a successful pregnancy. IVF is one of several assisted reproductive technologies (ART) designed to address infertility issues, differing from other methods in key ways. While IVF is often the first treatment option considered, it is important to understand its distinctions from other techniques. For instance, IUI, or intrauterine insemination, is a less invasive procedure that places sperm directly into the uterus during ovulation, aiming to enhance the chances of natural fertilization. Unlike IVF, IUI does not require egg retrieval or laboratory fertilization and can be a less invasive and more cost-effective option. However, IUI may be less effective in cases of severe male infertility or other significant fertility challenges. CureValue . ICSI is often used in conjunction with IVF, particularly when sperm quality or quantity is an issue. This method involves the direct injection of a single sperm into an egg to facilitate fertilization. While ICSI shares the egg retrieval and embryo transfer stages with IVF, its approach to fertilization is unique. The decision to use IVF with conventional insemination or ICSI depends on the specific fertility challenges faced by the couple and the likelihood of achieving successful fertilization through each method. In summary, IVF is a multifaceted and highly regulated process, integral to addressing infertility, and is supported by various ART techniques tailored to meet the unique needs of individuals and couples seeking to conceive.
The IVF process is not only technical but also deeply emotional, as it often represents hope for many couples facing infertility. Each step is accompanied by physical, psychological, and financial considerations that can significantly impact patients' experiences. The hormonal treatments required for ovarian stimulation can lead to side effects, such as mood swings, bloating, and discomfort, which necessitate thorough communication between patients and healthcare providers. Support systems, including counseling services, can help patients navigate the emotional rollercoaster of treatment, offering coping strategies and emotional support throughout their journey.
In addition to emotional support, financial transparency is crucial in the IVF process. Costs can vary significantly depending on factors such as geographical location, the specific clinic's pricing, and whether additional treatments like ICSI or genetic testing are required. Many patients are not aware of the full range of expenses involved, including medications, laboratory fees, and potential travel costs for those seeking treatment abroad. It's vital for clinics to provide clear information about pricing, payment plans, and insurance coverage options to help patients make informed decisions.
Understand the Process: Familiarize yourself with each step of the IVF journey, from stimulation to embryo transfer.
Choose a Reputable Clinic: Research clinics with high success rates and positive patient reviews.
Consult a Specialist: Meet with a fertility specialist to discuss your options and any underlying issues.
Lifestyle Changes: Adopt a healthy lifestyle—balanced diet, regular exercise, and avoiding smoking and excessive alcohol.
Manage Stress: Practice stress-reduction techniques like yoga, meditation, or mindfulness to support emotional well-being.
Follow Instructions: Adhere to your doctor’s medication and lifestyle instructions during the stimulation phase.
Track Your Cycle: Keep a detailed record of your menstrual cycle to aid in treatment planning.
Consider Genetic Testing: Discuss Preimplantation Genetic Testing (PGT) to screen for genetic disorders in embryos.
Stay Hydrated: Drink plenty of water to help your body respond well to medications.
Get Support: Seek emotional support from friends, family, or support groups to navigate the emotional ups and downs.
Know the Costs: Understand the financial aspects of IVF, including insurance coverage and potential additional costs.
Prepare for the Waiting Game: Be ready for the emotional challenges during the two-week wait after embryo transfer.
Stay Open to Options: Be open to different paths, including donor eggs, sperm, or surrogacy, if needed.
Monitor Your Health: Regularly check in with your healthcare provider about any side effects or concerns during treatment.
Limit Caffeine: Reduce caffeine intake, as high consumption may impact fertility.
Maintain a Positive Mindset: Stay hopeful and focused on the potential positive outcomes.
Communicate with Your Partner: Keep the lines of communication open with your partner to support each other emotionally.
Learn About the Medications: Familiarize yourself with the medications you’ll be taking and their side effects.
Plan for Follow-Up: Prepare for follow-up appointments to monitor progress and discuss next steps.
Celebrate Small Wins: Acknowledge and celebrate milestones along the way, regardless of the outcome.
Furthermore, the success rates of IVF can vary based on numerous factors, including the age of the woman, the underlying cause of infertility, and the quality of the eggs and sperm. Clinics typically provide statistics on success rates based on age and specific treatments, allowing patients to understand their chances of achieving pregnancy through IVF. This data can empower patients to set realistic expectations and make informed choices regarding their reproductive options.
The advancements in technology continue to enhance the IVF process, making it more effective and accessible. Innovations such as preimplantation genetic testing (PGT) allow for the screening of embryos for genetic disorders before implantation, helping to ensure healthier pregnancies. Additionally, improvements in cryopreservation techniques enable clinics to freeze embryos for future use, offering patients greater flexibility in family planning.
For those considering IVF, it is essential to choose a reputable fertility clinic with a track record of success and a supportive environment. Patients should research various clinics, read reviews, and seek recommendations from healthcare professionals or support groups. It's also beneficial to schedule consultations with potential providers to discuss treatment options, success rates, and the overall approach to patient care.
CureValue .
Ultimately, IVF is a complex journey that requires careful consideration, thorough planning, and strong support systems. While it presents challenges, the potential rewards-such as the joy of parenthood-make it a worthwhile path for many. As the landscape of reproductive medicine continues to evolve, IVF remains a beacon of hope for countless individuals and couples striving to build their families.
Preimplantation Genetic Testing (PGT) is another advanced technique that can be used alongside IVF. PGT involves analyzing embryos for genetic abnormalities before implantation to increase the chances of a healthy pregnancy. This method can be particularly valuable for individuals with known genetic disorders or advanced maternal age. While PGT enhances the IVF process by providing additional insights into embryo health, it is not a standalone treatment but rather an adjunct to the IVF procedure.
Gamete Cryopreservation, which includes egg and sperm freezing, is another ART method that complements IVF. Cryopreservation allows for the preservation of reproductive cells for future use, which can be beneficial for individuals who wish to delay childbearing or for those undergoing medical treatments that may affect fertility. IVF (In Vitro Fertilization) . While cryopreservation itself does not involve fertilization or embryo transfer, it can be integrated with IVF when the time is right for conception.
Lastly, Egg Donation and Surrogacy are additional ART options that involve different considerations. Egg donation involves using eggs from a donor to be fertilized via IVF, which is an option for individuals with issues related to egg quality or quantity. IVF (In Vitro Fertilization) . Surrogacy, on the other hand, involves a surrogate carrying the pregnancy for another individual or couple. Both options can be used in conjunction with IVF to achieve pregnancy but involve additional legal, ethical, and logistical considerations.
Overall, while IVF is a foundational ART method with a broad application, other techniques like IUI, ICSI, PGT, and gamete cryopreservation offer additional options and specialized approaches to address various infertility issues. Each method has its own indications, benefits, and limitations, and the choice among them depends on individual circumstances, fertility diagnoses, and personal preferences.
The process of In Vitro Fertilization (IVF) involves several crucial steps, each carefully designed to maximize the chances of a successful pregnancy. Understanding these steps provides insight into the meticulous nature of the IVF treatment cycle and highlights the complexity of assisted reproductive technology.

The IVF treatment cycle begins with ovarian stimulation, where the individual undergoing treatment receives hormone injections to stimulate the ovaries. The goal is to encourage the development of multiple follicles, each containing an egg, rather than the single egg typically produced in a natural cycle. This phase usually lasts about 8 to 14 days, during which the response to the medication is closely monitored through blood tests and ultrasound imaging. Monitoring ensures that the eggs are developing properly and helps determine the optimal time for the next phase.
Once the follicles have matured, the next phase is egg retrieval or aspiration, a crucial step in the IVF process. This procedure is conducted under sedation or anesthesia to ensure the patient's comfort and minimize any potential discomfort. A thin, hollow needle is carefully guided through the vaginal wall and into the ovaries, utilizing real-time ultrasound imaging for precision. This technique allows the clinician to aspirate the mature eggs directly from the follicles. Once retrieved, the eggs are sent to the laboratory for thorough evaluation, where their quality and readiness for fertilization are assessed.
Following egg retrieval, the fertilization process begins. In the lab, the mature eggs are combined with sperm to facilitate fertilization. This can be accomplished through conventional insemination, where sperm is introduced to the eggs and allowed to fertilize naturally, or via Intracytoplasmic Sperm Injection (ICSI), a technique that involves directly injecting a single sperm into each egg. The choice between these methods is influenced by several factors, including sperm quality and the specific underlying causes of infertility.
Once fertilization occurs, the embryos enter the culture stage, which typically lasts about 3 to 5 days. During this time, embryologists closely monitor the embryos' development, evaluating their growth and selecting the most viable candidates for transfer. The objective is to encourage the embryos to reach the blastocyst stage, which is optimal for implantation into the uterine lining.
The next critical step is the embryo transfer, where one or more selected embryos are placed into the uterus. This procedure is usually performed without anesthesia and involves inserting a thin catheter through the cervix to deposit the embryos into the uterine cavity. Timing is essential; the transfer is generally scheduled to occur 1 to 2 days after the embryos reach the blastocyst stage to maximize the chances of successful implantation.
After the embryo transfer, patients often receive hormonal support, typically in the form of progesterone supplements. This support is vital for maintaining the uterine lining and creating an environment conducive to embryo implantation and early pregnancy. Hormonal support helps optimize the uterine lining, ensuring it is receptive to the developing embryo.
CureValue allows users to compare options from a wide range of trusted facilities worldwide and access verified profiles of doctors and medical centers.
Patients can join CureValue by seeking treatment through their platform and becoming part of their community dedicated to making healthcare better for everyone.